The gist of science is nothing more than a refinement of everyday life!
Over the past few years, our health system is moving forward to care for patients with severe wounds or ulcers with the hope to be back to life again. These wounds are generally aftereffects of some kind of infections and there are various reasons why we can get affected by it such as injuries, cuts, burns or poor circulation, etc. There are some vascular illnesses such as diabetes, which can cause wounds affecting the structural and functional integrity of the skin.
The skin is the largest yet practically ignored organ of our body. It protects us from various environmental pathogens, that can be harmful to our bodies. Just imagine our body, without skin and all our organs are exposed to the outer environment! Terrifying, isn’t it? This natural barrier is made up of three integral layers known as the epidermis that’s the outermost layer, the dermis that’s the middle one, and the deepest being hypodermis. The epidermal layer is made up of four different types of cells, namely keratinocytes for the protein keratin imparting water-resistant quality, Merkel cells for detecting sensation, Langerhans cells to get rid of debris thereby preventing the infection, and melanocytes that impart color to the skin. The middle dermal layer is made up of fibroblasts, blood vessels, skin appendages that are attached together to support the cells. As with the epidermis even these dermal components determine their function. Blood vessels nourish skin, immune cells protect the cells and fibroblasts make collagen form strength and elasticity. Similarly, the deepest hypodermis acts as a cushion to protect underlying bones, muscles, and tendons. Being a fatty tissue, it is made up of many adipocytes to regulate skin homeostasis and the growth of cells within the skin appendages.
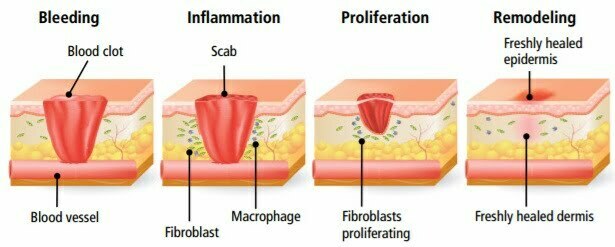
You must have wondered many times, as to how a small cut or mark on the skin can disappear after some days. The explanation can be that the skin is actually the powerhouse of regeneration. As the upper layer of skin cells, when ones found on the surface are all dead cells, when they are sloughed off, new cells from underneath move up to replace them. The process is regulated by the deepest tissue hypodermis, which is made up of many stem cells. Wound develops when the epidermal layer of the skin is disrupted by the injury or burn and with the involvement of deep layers the severity of the disease is increased. However, our skin has a normal healing mechanism involving inflammation, proliferation, and remodeling. In this regard, the keratinocytes play a major role in the restoration of the epidermis and the formation of a new layer as an interface between the epidermis and the dermis. Although as in the case of deep wounds, these keratinocytes are destroyed, and hence the fewer number of them are available for repairing and restoring the damage. As a result of which deep wounds are taking a long time to heal.
Undoubtedly the treatment options for these patients are available with good quality care involving skin grafting. But these treatments generally come with the package of poor regeneration of the skin or leaving behind scar tissue or unavailability of suitable skin grafts, dry itchy skin, etc. Thus the success ratio for these treatments can just be 50%. Albeit there is a new treatment option available at our fingertips that can fundamentally change burn treatment delivery, Stem cell treatment for wound healing.
These masters cells are actively explored for wound therapy due to their enormous potential to differentiate into any cells of the body, especially various components of skin cells. These cells can be able to regulate the physiological process for maintaining structural and functional integrity of tissue and thereby organs. With the advanced scientific methodology, we can be able to scientifically guide these cells to be the desired cell types, keratinocytes, and other epidermal cells in the case of skin tissues. This power, we all have within us. A potential to regenerate lost tissues with the use of stem cells. We all have a reserved number of stored stem cells quota with us in sources such as Adipose tissue or Bone Marrow, which can be isolated in the laboratory and implanted back into the patient’s wound to be the desired skin cells. These cells can be keratinocytes, fibroblasts, fat cells, such as Adipocytes which will be able to restore skin layers somewhat near to the natural process. Being isolated from your own body, there is a minimum risk of rejection and availability. A number of studies have been completed using bone marrow isolated autologous stem cells in severely burnt or wound patients, resulted in complete healing of the wound.
Thus, with the advances in medicine, stem cells do offer a realistic alternative to conventional medicine with the ability to naturally heal chronic wound.


Recent Comments